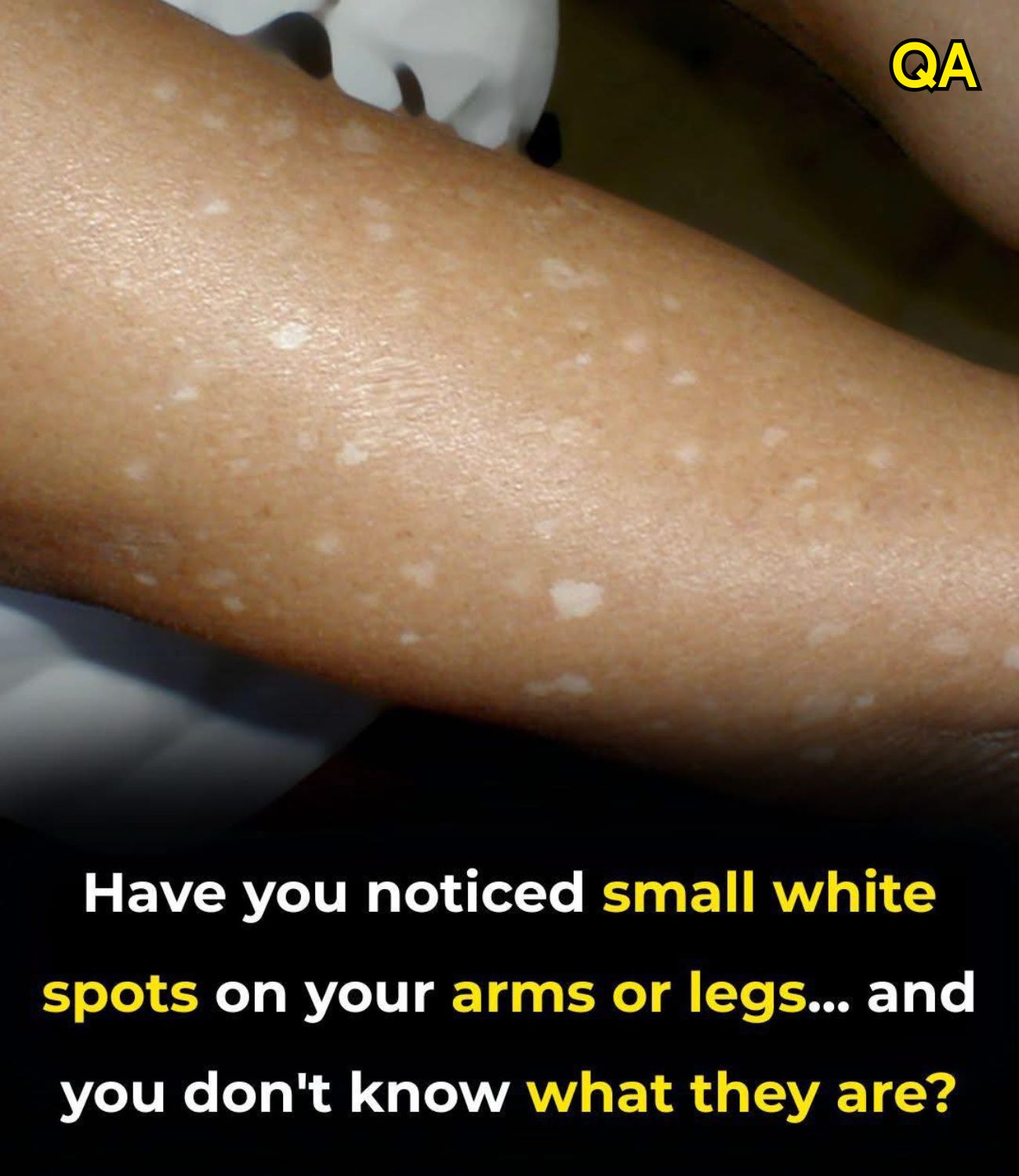
As the last traces of a summer tan begin to fade and the cooler months settle in, many people find themselves noticing something they had not paid much attention to before: small, pale dots appearing on their legs and arms. These tiny white marks tend to stand out more clearly against the slightly darker surrounding skin, and because they become more visible as a tan recedes, autumn and winter are often when people first become genuinely aware of them. For some, the spots appear to multiply with each passing year, showing up in new locations and in greater numbers, leading to a natural combination of confusion and quiet concern.
If you have looked down at your arms or legs and found yourself wondering what these little pale patches are, where they came from, and whether they signal something that needs medical attention, you are far from alone. The question is one of the most commonly searched skin-related queries online, and the answer — for the vast majority of people — is considerably more reassuring than the initial sight of the spots might suggest.
What Exactly Are These White Spots?
The condition most commonly responsible for these small pale marks is known medically as idiopathic guttate hypomelanosis, a term that is typically abbreviated to IGH. The name sounds considerably more alarming than the condition itself warrants. Broken down into its component parts, the term simply describes spots (“guttate” comes from the Latin for droplet) of reduced pigmentation (“hypomelanosis”) whose precise origin is not entirely understood (“idiopathic,” meaning arising spontaneously without a clearly identified cause).
In practical terms, IGH refers to small, flat, white or very pale patches of skin that appear due to a reduction or complete local loss of melanin — the pigment that gives human skin, hair, and eyes their color. The spots are typically only a few millimeters in diameter, though they can occasionally be slightly larger. They are smooth to the touch, have well-defined edges, and do not cause any physical discomfort. They do not itch, do not crust over, do not weep, and do not change in texture. They simply appear — small, pale, and permanent — and tend to stay exactly as they are for years or decades without any meaningful change in their character.
IGH can appear on people of every skin tone and ethnic background, though the spots tend to be most visually noticeable on people with medium to darker complexions, where the contrast between the pale spot and the surrounding skin is most pronounced. The areas of the body most commonly affected are those that receive the most regular sun exposure: the forearms, the shins, the upper arms, and occasionally the face and the back of the hands. They are considerably less common on areas of the body that are typically covered by clothing.
One of the most important facts about IGH is simply how common it is. Dermatological research suggests that somewhere between fifty and eighty percent of people over the age of forty will develop at least a handful of these spots at some point. By the time a person reaches their sixties or seventies, having a significant number of them across the arms and legs is entirely typical. They are, in the most straightforward sense, a normal and extremely prevalent feature of aging human skin.
Why Do These Spots Appear? Understanding the Underlying Mechanism
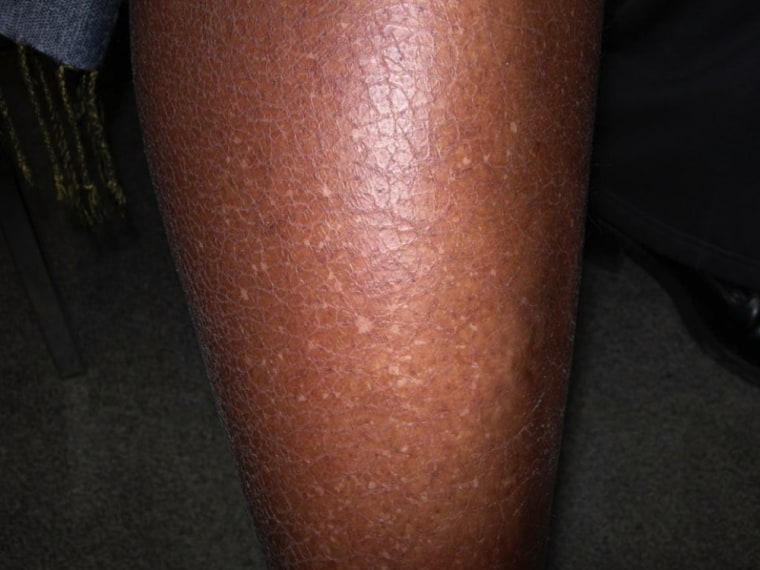
To understand why IGH develops, it helps to understand a little about how skin color is produced in the first place. The color of human skin is determined primarily by the activity of specialized cells called melanocytes, which are distributed throughout the deepest layer of the skin’s outer covering. Melanocytes produce melanin, which they then transfer to surrounding skin cells, where it accumulates and creates the visible color we associate with a person’s complexion. When the skin is exposed to ultraviolet radiation from sunlight, melanocytes increase their melanin production — which is why skin darkens in response to sun exposure.
Over a lifetime of sun exposure, however, the cumulative effect of ultraviolet radiation begins to take a toll on melanocytes. The DNA within these cells sustains damage over time, and in some locations this damage eventually causes the melanocytes to malfunction or cease functioning altogether. When the melanocytes in a small area of skin stop producing melanin effectively, that area no longer has access to pigment — and it appears lighter than the surrounding skin, creating the pale spot that characterizes IGH.
This explains several of the condition’s most notable features. It explains why the spots appear most frequently on sun-exposed areas of the body rather than on covered skin. It explains why they become more numerous with age, since the accumulated damage to melanocytes increases over time and more cells are progressively affected. And it explains why they are essentially permanent — once a melanocyte has been sufficiently damaged to stop producing melanin, it does not simply recover and resume normal function.
The process is gradual and cumulative, which is why people rarely notice a sudden appearance of many spots at once. Instead, a person might have three or four spots in their thirties, a dozen or more in their forties, and a considerably larger number by the time they reach their sixties. Each spot marks a small location where the cumulative burden of ultraviolet damage finally exceeded what a local cluster of melanocytes could sustain.
It is worth noting that while sun exposure is the primary and most well-established contributing factor, some researchers have suggested that genetic predisposition may also play a role in determining how susceptible any individual person’s melanocytes are to this kind of cumulative damage. People whose parents or grandparents developed prominent IGH spots may be somewhat more likely to develop them as well, though the relationship is not straightforward enough to be predictive in any meaningful clinical sense.
Is IGH Dangerous? What You Actually Need to Know
The most important thing to understand about idiopathic guttate hypomelanosis is that it is a benign condition. It does not indicate the presence of any underlying disease. It is not associated with increased risk of skin cancer or any other serious medical condition. It does not spread in the way that infections spread, does not affect any internal organ or system, and does not represent a malfunction of the immune system. The spots are simply areas where melanocytes have ceased to function adequately — nothing more complicated or alarming than that.
This is genuinely reassuring information for the large number of people who discover these spots and immediately begin searching for explanations, sometimes arriving at concerning possibilities before finding the more mundane and accurate answer. IGH is not a warning sign. It is a feature of aging skin, as normal in its own way as gray hair or the fine lines that develop around the eyes over the course of a lifetime.
That said, it is always reasonable to have any new or changing skin feature examined by a qualified dermatologist, particularly if you notice spots that are growing rapidly, changing shape or color, developing irregular borders, becoming raised or thickened, or producing any kind of physical sensation such as itching or tenderness. These features would suggest that something other than IGH might be responsible, and a professional assessment would provide clarity. IGH spots themselves, once established, tend to remain stable and consistent over time. Spots that are behaving differently from this pattern deserve professional attention.
Could These Spots Be Something Else? Distinguishing IGH from Other Conditions
Several other skin conditions can produce pale or white spots on the skin, and it is worth being aware of how they differ from IGH.
One commonly confused condition is tinea versicolor, a skin condition caused by an overgrowth of a type of yeast that naturally lives on the skin surface. Tinea versicolor can produce patches of skin that appear lighter than the surrounding area, particularly on the chest, back, and shoulders. However, these patches tend to have a slightly different quality from IGH — they may have a faintly scaly or powdery texture when examined closely, they sometimes cause mild itching, and they respond to antifungal treatments, which IGH does not. The distribution is also typically different: tinea versicolor tends to favor the trunk rather than the limbs, and its patches are often larger and more irregular in shape than the neat, small dots of IGH.
Another condition that produces depigmented patches is vitiligo, which involves a more extensive and often progressive loss of pigmentation affecting larger areas of skin and sometimes appearing on the face, hands, and other visible areas. Vitiligo patches tend to be larger, more irregular, and more rapidly expanding than IGH spots, and the condition has a different underlying mechanism involving the immune system rather than sun-induced damage. A dermatologist can readily distinguish between the two.
Post-inflammatory hypopigmentation — pale patches left behind after the resolution of certain skin conditions or injuries — can also occasionally be confused with IGH, though the history of a preceding skin event usually provides the necessary context for correct identification.
The key distinguishing features of IGH remain its small size, its smooth flat surface, its location on sun-exposed limbs, its stability over time, and the complete absence of any associated symptoms.
Can These Spots Be Treated or Removed?
This is the question that most people arrive at fairly quickly once they understand what IGH is. The honest and somewhat disappointing answer is that there is currently no treatment that has been shown to permanently and reliably restore normal pigmentation to areas affected by IGH.
A range of approaches have been explored and are sometimes discussed or marketed in various contexts. Topical retinoid creams, which promote skin cell turnover and have proven benefits for other aspects of skin aging, have been tried with inconsistent results in IGH. Chemical peels, which remove the outer layers of skin and stimulate renewal, have similarly shown limited and unpredictable outcomes. Various laser and light-based therapies have been investigated, with some producing temporary improvements in individual cases, but none demonstrating the kind of consistent, lasting restoration of pigmentation that would justify recommending them as standard treatment.
The fundamental challenge is biological: once the melanocytes in a given area have been damaged to the point of dysfunction, the therapeutic options for restoring their activity are genuinely limited. Melanocytes are not cells that regenerate readily in the way that some other cell types do, and the mechanisms for reactivating damaged ones in a reliable and lasting way are not yet well understood at a clinical level.
For this reason, most dermatologists do not actively recommend treatment for IGH as a medical matter, since the condition itself poses no health risk and the available interventions offer limited cosmetic benefit at meaningful cost and sometimes with their own risk of side effects or complications.
Practical Steps for Managing IGH Cosmetically and Preventing New Spots
While the spots themselves cannot be reliably eliminated, there are practical approaches that many people find helpful for managing their appearance or preventing additional spots from forming.
Daily application of broad-spectrum sunscreen to sun-exposed areas of the skin is the single most important step a person can take — both to slow the rate at which new spots appear and to protect the skin from the broader range of sun-related damage that accumulates across a lifetime. Sunscreen with an SPF of thirty or higher, applied generously and reapplied after swimming or prolonged outdoor activity, provides meaningful protection for the melanocytes that are still functioning normally and reduces the pace at which new ones sustain damage.
For people who find the appearance of the spots bothersome in a cosmetic sense, body makeup formulated for the skin on arms and legs can effectively even out the skin tone for occasions when this matters. Similarly, self-tanning products can temporarily reduce the contrast between the pale spots and the surrounding skin, making the spots less visually prominent — though this effect fades as the product is metabolized and washed away.
Keeping the skin well moisturized does not change the underlying pigmentation situation but does improve the overall texture and appearance of the skin in ways that many people find make the spots somewhat less noticeable in daily life.
A Final Word: Reassurance and Perspective
Perhaps the most useful thing to take away from all of this is simply a shift in perspective. The small pale spots that appear on aging skin are not a sign of illness, not a warning, and not something that requires urgent action. They are a normal, extremely common, and entirely harmless feature of skin that has lived in the world for several decades, absorbing sunlight and doing the remarkable work that skin does every day without acknowledgment.
They are, in the most literal sense, marks of a life lived — small visible records of summers spent outdoors, of years accumulated, of time passing in the way that time does. Understanding what they are makes them considerably less alarming, and for most people, that understanding is exactly the reassurance they were looking for when they first noticed them and began to wonder.
If you are ever uncertain about any skin change — whether because of its appearance, its behavior over time, or simply because something about it feels different from what is described here — a conversation with a qualified dermatologist will always provide the most reliable and personalized guidance. But for the vast majority of people who have found these small pale dots on their arms and legs and come looking for an explanation, the answer is a simple and genuinely comforting one: this is normal, this is common, and you are fine.